News
Members
Publications
Software / Data
Job offers
Images / Videos
Collaborations
Conferences
Lab meetings: "Les partages de midi"
Practical information
Members Area
Next conferences we are in …



This is an old revision of the document!
See also the ACouStiC web site: ANR Blanc grant for 4 years starting in 2011 - PI: P. Jannin
Stimulation is a minimally invasive therapy, which was developed for various diseases more than 20 years ago and is currently emerging as a powerful tool with increasing potential. We will address common aspects related to stimulation procedures, such as model supported surgical planning, intraoperative imaging for helping implantation in the OR, and postoperative assessment based on images and clinical scores. Parkinson Disease (PD) prevalence is about 1% in adults over 60 years old. High frequency Deep Brain Stimulation (DBS), also considered as a brain pacemaker, has been demonstrated as an efficient minimally invasive surgical treatment for treating Parkinson or motor related diseases and recently severe neuropsychological diseases. It was originally developed in France by Pr. Benabid (Grenoble).
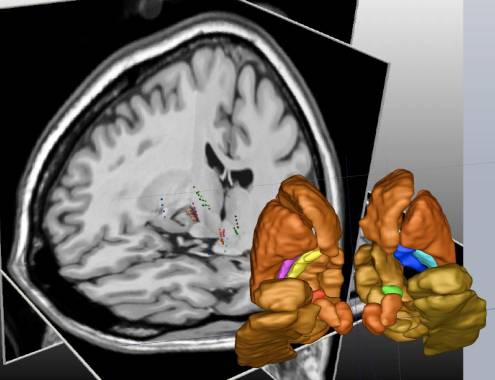
As demonstrated in the literature, the quality of the clinical improvement, as well as the existence of motor, neuropsychological or psychiatric post operative side effects strongly depend on the location of the electrode, and therefore on the quality of the surgical planning.
The main objective of our project, funded by a ANR Blanc grant for 4 years starting in 2011 (Acoustic ), is to develop an innovative strategy based on models for helping decision-making process during surgical planning and post operative assessment in DBS for increasing the accuracy and precision of DBS. Two types of models will be made available to the surgeon: patient specific models and generic models. We will study methods for building 1) patient specific models from multimodal medical images dedicated to DBS and 2) generic anatomo-clinical models that gather location of the electrodes and clinical scores from a population of patients. Histological atlases will also be available thanks to collaboration with the CRICM (Centre de Recherche de l'Institut du Cerveau et de la Moelle) – UPMC / INSERM UMR_S975 / CNRS UMR 7225 Pitié-Salpêtrière Hospital in Paris. Dedicated linear and non-linear image registration methods will be developed with the CRICM. Strategies for building the anatomo-clinical atlases will be studied as well as strategies for extracting rules from these models defining optimal targets for DBS.
Secondly, the project will develop methods for automatic computation of optimal electrodes trajectories from these models, taken into account the rules expressed by the surgeons, the knowledge available in the atlases, and the patient specific data and information thanks to collaboration with the IGG team (Geometrical and Graphical Informatics) of LSIIT (Image Sciences, Computer Sciences and Remote Sensing Laboratory) from the University of Strasbourg. For better accuracy and precision, we will also simulate the possible deformations of the final electrode and anatomical structures during surgery and integrate this simulation into the trajectory computation thanks to collaborations with the ALCOVE INRIA team in Lille.


